Diabetes is not a single disease; it’s a group of many diseases. All the diseases are lump together and cause diabetes mellitus. It is a metabolic de-arrangement in our body. This is a group of metabolic diseases that are put together due to some common disease. That common disease is a tendency for chronic hyperglycemia and reduced insulin production. In hyperglycemia either there is increase resistance to the action of insulin or there is reduce the production of insulin.
How does diabetes occur?
We can understand by there are pancreas and beta cells that produce insulin that is going through the blood to the cells and act on its receptors. But, when production reduces or action reduces or both things occur like reduced production or increased resistance which makes diabetes a very big problem.

In this group of diseases there are many different types of diabetes which are as follows:
Type 1 diabetes:
This is a classical example of diabetes mellitus. In this, there is a severe reduction in the production of insulin, or sometimes absolutely absent because beta cells that produce insulin are attacked by the immune system or we can say that beta cells are destroyed due to an autoimmune reaction.
Type 2 diabetes:
Type 2 diabetes is a major problem. In this resistance to the action of insulin at least in the initial stages because the beta cells of the pancreas might be producing insulin at a normal level or more than normal but cells are not responding to insulin.
Gestational diabetes:

This is a condition in which during pregnancy there is a tendency for hyperglycemia or there is hyperglycemia. In this condition, there is a problem in the production of insulin as well as there is peripheral resistance that tissues are not responding well to the insulin.
LADA (latent autoimmune diabetes of adults):
LADA stands for “latent autoimmune diabetes of adults”. In this condition, the immune system attacks beta cells in the pancreas at a slower rate compared to type 1 and type 2 diabetes.
It develops most commonly in people over 30 years old. because of which it is misdiagnosed. Because some healthcare experts still think that type 1 diabetes occurs only during childhood.
Medication and lifestyle changes can help in treating LADA for some years. But after some time as insulin production declines, insulin becomes as compulsory as your daily health management for type 1 diabetes.
Signs and symptoms of LADA:
They include symptoms of both type 1 and type 2 diabetes. Some of the primary symptoms are:
- Difficulty in concentration (brain fog)
- Itchy skin, dryness
- Constant feelings of tiredness and lethargy
- Feeling hungry all time
As the problem raises more, the more symptoms you will develop:
- Feeling thirsty constantly
- Frequent urination
- Vision changes
- Tingling in hands, feet, and legs
- Tired or exhausted all time
- Lose weight unexpectedly
- Yeast infection (in women)
Factors to diagnose LADA:
The age is over 30 years of patients.
At least one out of four types of tests is positive for diabetes-related autoantibodies.
There is no requirement for insulin for at least six months after their initial diagnosis.
Another autoimmune diseases including Grave’s disease, celiac, or Hashimoto’s disease can be present.
Types of tests to diagnose LADA:
- (GAD) Glutamic acid decarboxylase
- (ICAs) Islet cell antibodies
Some other tests also can help in the diagnosis of LADA:
- (HbA1c) Haemoglobin A1c test
- (FPB) Fasting plasma glucose test
- (OGTT) oral glucose tolerance test
- Ketone test
Treatment of LADA:
- Daily insulin therapy
- Blood sugar monitoring
- Food choice
Maturity onset diabetes of young people (MODY):
In this type of diabetes, there are symptoms of type 2 diabetes but it occurs at a younger age. In MODY, the body’s ability to produce insulin is limited but different than type 1 diabetes. When there is a decrease in insulin production, blood glucose level raises which causes diabetes.
Signs and symptoms:
MODY symptoms develop slowly, so it is possible to have no symptoms at first. That is why MODY is often left undiagnosed for a long time. Symptoms are:
- Skin infection
- Yeast infection
- Urinating frequently
- Thirsty frequently
- Blurred vision
Causes of MODY:
MODY is caused by a single gene mutation which is why it is a “monogenic” disease. A different gene mutation can cause MODY. If someone has a family member with MODY, then they have an increased risk for the condition.
Diagnosis of MODY:
Different types of tests can help in the diagnosis of MODY:
Blood sugar test- this is the first step for diagnosing MODY. If these test results are positive then a doctor can advise you further test to assess the type of diabetes you have.
Genetic test- MODY occurs due to genetic mutation; a genetic test can help in the diagnosis of MODY.
Treatment of MODY:
Treatment is done with oral medications or insulin injections. Some forms don’t need any treatment. The treatment varies depending on what genetic mutation caused the condition.

Complications of diabetes mellitus:
Diabetes causes a lot of disturbances in a person’s body. It not only causes disturbance in carbohydrate metabolism but also lipid metabolism and protein metabolism. Complications of diabetes are divided into two categories:
Long-term complications-
Also, diabetes can produce vascular problems which we consider a disease also because it has various complications in it.
Diabetes damages the vessels (the vascular disease) and angiopathy are into two types:
- Big vessel diseases (macrovascular complication) or macro angiopathy
- Small vessel diseases (microvascular complications) or microangiopathy
Macrovascular complications:
They occur from changes in the medium to large blood vessels. The blood vessel walls get thick, sclerosis, and become occluded by plaque that adheres to the vessel walls. So, the blood flows is block.
The macrovascular complication occurs due to damage to larger blood vessels. These complications can occur in the blood vessels of any body part. They include diseases of coronary arteries, peripheral arteries, and cerebrovasculature. The early stage is associated with an atherosclerotic plaque in the vasculature supplying blood to the heart, brain, limbs, and other organs. The late step involves complete obstruction of these vessels which can cause myocardial infarction (MI), stroke, claudication, and gangrene.
Peripheral arterial disease
It is present in approx 29% patients of with diabetes and may remain undiagnosed due to lack of sensation because of neuropathy to identify pain.
Symptoms- claudication, ulcers, limb amputation
Screening and prevention – as part of a thorough history, patients ask about foot ulceration as well as limb claudication. Screening of all patients with diabetes over the age of 50 years is recommended with Ankle Brachial Index (ABI).
Coronary Heart Disease
Patients with type 2 diabetes are at an equal risk of getting myocardial infarction as well as patients with Coronary Heart Disease. Almost 75% of patients with diabetes are most probably having obstructive or non-obstructive coronary artery disease also.
Screening and prevention – However, the patient should be screened every year for being overweight or obese, hypertension, dyslipidemia, tobacco use, chronic kidney disease, albuminuria, and a family history of coronary heart disease. If any of them are present, they should be managed appropriately.
Hypertension
An ideal range for blood pressure is 120/80 mmHg. Treatment for hypertension with a goal blood pressure of <140/90 mmHg for those with lower cardiovascular risks, and<130/80 mmHg for those with higher cardiovascular risks should be initiated. The beginning of treatment should be with angiotensin-converting enzyme (ACE) inhibitors or angiotensin receptor blockers (ARB) if albuminuria is present.

Lipid management
Patients over the age of 40 should start taking a statin, in addition to lifestyle modification. Also, the general recommendation is to use moderate-intensity statin for patients without CVD. For patients with multiple risk factors, a high-intensity statin is recommended.
Stroke
As diabetes increases the risk of coronary heart disease, the risk of stroke increases. It is higher in females than males. However, patients with type 2 diabetes have a high proportion of ischemic stroke from hemorrhagic stroke compared with the general population.
Screening and prevention:
Currently, there are not any guidelines present for patients with diabetes. However, in patients with other diseases or cardiovascular risk factors, there may be benefits. The patient should have strict blood glucose control.
Microvascular complication-
The microvascular complication occurs by the damage of smaller vessels. They include neuropathy, nephropathy, and retinopathy.
Retinopathy-
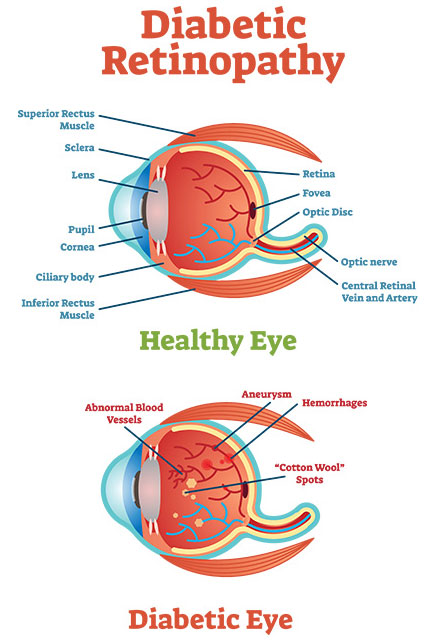
It is one of the leading causes of vision loss worldwide and is the main cause of blindness in working-age adults in the USA. Initially, there are no symptoms until the extremely late stages. Although, the primary risk factors for diabetic retinopathy development are the duration and intensity of glycemic control. Uncontrolled hypertension, hyperlipidemia, and the presence of other complications such as diabetic nephropathy and neuropathy worsen the underlying retinopathy. We have to also control these risk factors for the prevention of diabetic retinopathy.
Prevention-
For diabetic patients, enhancing glycemic control and treatment of systemic conditions like hypertension and hyperlipidemia is essential to prevent vision loss. Also, various studies have proven that lowering glycated hemoglobin reduces the rate and progression of diabetic retinopathy. Prevention is done by the following methods –
- Blood pressure control
- Cholesterol-lowering therapy
- Exercise
Neuropathy-

Diabetic patients are also affected by neuropathies. There are two main neuropathies
- Distal symmetric polyneuropathy – The presence of symptoms of peripheral nerve dysfunction in people with diabetes after the exclusion of other causes. This is because of inflammatory stress or oxidative stress which leads to the damage of nerve cells. However, patients with type 2 diabetes should check for distal symmetric polyneuropathy once a year, and with type 1 diabetes, in 5 years. Screening is done by taking a thorough history and examination of the patient. The patient may feel numbness and tingling and sometimes pain.
- Cardiovascular autonomic neuropathy – symptoms of this condition are hypoglycemia, orthostatic hypotension, gastroparesis, Bowel irregularities erectile dysfunction, and other autonomic deregulations. Also, cardiovascular autonomic neuropathy is not present in early diabetes. It increases with time. Symptoms are lightheadedness, faintness n palpitations, or syncope. Variability in heart rate while standing is also an indicator of cardiovascular autonomic neuropathy
- Other neuropathies – Neuropathic patients should also be screened for gastroparesis. by asking about symptoms like nausea, early satiety, or unexpected glycemia variations. Also, every patient with neuropathy should check for lower urinary tract symptoms such as incontinence and bladder dysfunction. Female sexual dysfunction including less libido, dyspareunia, and inadequate lubrication should screen.
Nephropathy –

Although, nephropathy is common in patients with type 1 and type 2diabetes. It is 20 – 40% prevalent in patients with diabetes. the presence of reduce glomerular filtration rate (GFR) or increase urinary albumin excretion for at least 3 months in a diabetic patient.
Screening – screening is done once a time in a year on a patient with type 1 diabetes and five years on a patient with type 2 diabetes
If micro albumin urea is present then non-diabetic conditions causing albumin urea like urinary tract infection, haematuria, heart failure, febrile illness, severe hyperglycemia, and heavy exercise should be done more.
Prevention and treatment –
- Lifestyle modification
- Healthy eating
- Exercise regularly
- Weight loss
Acute complication of diabetes:
Acute complication includes:
Hypoglycemia or insulin reactions-
In this condition blood glucose level falls less than 50-60 mg/dl because of too much insulin or oral hypoglycaemic agents, significantly less food intake, or over-physical activity.
This condition can occur at any time of day or night. Although, this is more common before meals or meals get delay or fasting.
There are two categories:
- Adrenergic symptoms- There is mild hypoglycemia because the blood glucose level falls, and the sympathetic nervous system stimulates, which causes a surge of epinephrine or norepinephrine.
Symptoms of mild hypoglycemia include- sweating, tremor, tachycardia, palpitation, nervousness, and hunger.
- Central nervous system symptoms- in this condition, there is moderate hypoglycemia which leads to a fall in glucose level which deprives the brain cells of needed fuel for normal functioning also.
Signs of impaired function of the CNS may include:
- Difficulty in concentration
- Headache
- Lightheadedness
- Memory lapse
- Confusion
- Slurred speech
- Impaired coordination
- Emotional changes
- Behavior changes
Severe hypoglycemia-
CNS function is impaired in hypoglycemia as the patient needs another person for treatment. Also, disoriented behavior, seizures, sleep problem, and low consciousness are symptoms of this condition.
Management of hypoglycemia:
The normal recommendation is 15 g of fast-acting, concentrated source of carbohydrates such as the following, given orally:
- 3-4 commercially prepared glucose tablets
- 4-6 oz of fruit juice or regular soda
- 6-10 hard candies
- 2-3 teaspoons of sugar or honey
If you are facing issues in dropping your weight, please take this free-body type assessment: Click here

